CX is all the rage these days. It seems that most of it is couched in theoretical theory and “potential” value creation. To be clear, we think it definitely has its purpose. In fact, it is core to our modelH approach. But, we are weary of anything that cannot be implemented in an Agile fashion.
In a McKinsey survey of senior executives, 90% said customer experience (CX) is one of the CEO’s top 3 priorities. This fact is due to increasing customer expectations in an evolving digital marketplace. Customers expect more, better and faster – and they expect you to know and fix your process problems. McKinsey research indicates that for every 10-point up in customer satisfaction, companies increase their revenues by 2 to 3%. Gains come from increasing wallet share (more product purchases) and lower churn rates (fewer customers leave). Satisfaction is correlated to operational or infrastructure-related factors. These include price, transparency, cycle times, product features, and use of digital channels.
We take for granted that the result of a great CX discipline produces customer action (behavior change), satisfaction (customer happiness), and attraction (brand loyalty). As a result, your employees will be able to understand how their work impacts the member’s experience – and establish a baseline for all future CX endeavors.
Though this seems straightforward, implementing a customer experience discipline within a company is difficult. So how do you begin?
Well, even the longest journey begins with a single first step. Experience is something that can be designed, implemented and measured. In healthcare, favorable experiences can make a difference between healthy/profitable customers and unhealthy/expensive ones. A better experience comes from orchestrating a customer’s journey across channels. Experiential design starts with recognizing and prioritizing your (i.e. your customer’s) most important “touches” so you can optimize the operational factors that drive them. For health plans, the inventory of touches includes your member as well as your providers.
We recommend you start with defining (in a minimally viable way) how the discipline of Customer Experience (CX) will work at your company. Although CX eventually encompasses all of your company’s touchpoints and communications, synchronized across channels to achieve maximum customer activation and brand awareness – we are asking you to just spend a day outlining the basics and assigning responsibility for them. Just do enough to define your most important first CX project(s) and get someone assigned to the task. Then see where it goes from there – and keep it Agile.
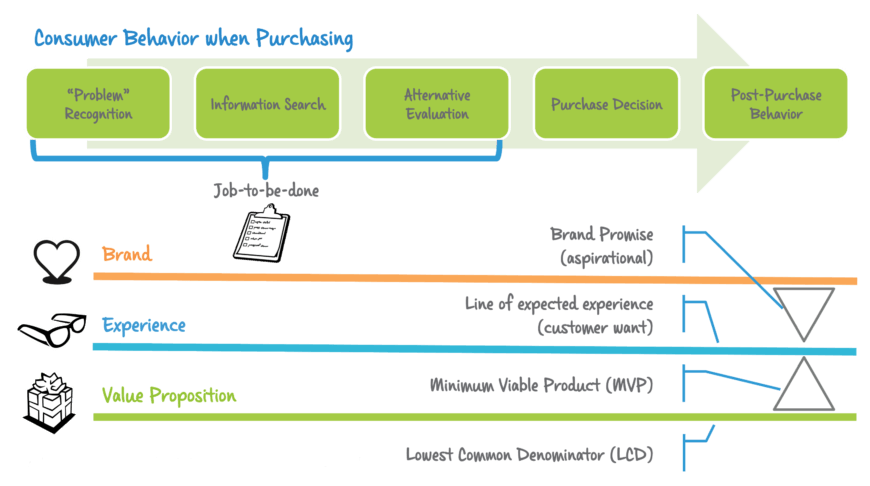
As first projects go, we recommend you start with a journey map. A Customer Journey Map is a graphic representation of the journey your prospect/customer takes in relationship to your organization over time and across all touch points. This tool emphasizes the intersections between your processes, your customer’s jobs-to-be-done, your measures, and your customer’s expectations. If you cannot define the touches, how can you truly prioritize which need fixing first? We recommend you first focus on the “experiences” that move the needle for customers and impact your cost/profit outlook. A few things stand out for prioritization. Digital journeys should be prioritized over manual ones as it easier to “fix” digital than physical. And, McKinsey research shows digital-first journeys produce higher customer-satisfaction scores than traditional journeys. Reducing journey time (the time it takes to complete an individual journey) should be prioritized over adding new features. Customer satisfaction has a higher correlation to “ease-of-use” than “feature rich”. However, keep in mind that there are diminishing payoffs for reducing journey time, so only take it as far as it produces returns.
imagine.GO specializes in helping companies thrive where consumerism and health care converge. We have helped organizations ranging from fortune-100 companies to startups, quickly define better business models and communicate them to stakeholders. We have implemented our “100 Days to Customer Experience” model for several large health insurance plans and other retail-focused healthcare companies.
Here is the link to the McKinsey article we are referencing (The four pillars of distinctive customer journeys).
To your health,
The Team at imagine.GO





















 So, my accelerometer of choice is the Nike+ FuelBand. Keep in mind, I tested most of the major brands: the FitBit Classic, the BodyMedia FIT LINK, and the Striiv Smart Pedometer. First, I wanted something that was simple. Second, I wanted something that was unobtrusive. Third, I wanted something I would remember to carry with me at all times. For these reasons I settled on the Nike+ FuelBand – however, I am not sure the Nike+ FuelBand is as accurate as the FitBit, as it seems to count movement that I do not consider exercise – like typing up a new BLOG.
So, my accelerometer of choice is the Nike+ FuelBand. Keep in mind, I tested most of the major brands: the FitBit Classic, the BodyMedia FIT LINK, and the Striiv Smart Pedometer. First, I wanted something that was simple. Second, I wanted something that was unobtrusive. Third, I wanted something I would remember to carry with me at all times. For these reasons I settled on the Nike+ FuelBand – however, I am not sure the Nike+ FuelBand is as accurate as the FitBit, as it seems to count movement that I do not consider exercise – like typing up a new BLOG.








